Bioethics Forum Essay
A Responsible Death
As debates continue about the decisions people make about how to die, I wish to draw wider attention to the death of Paul Drier, as reported in the Globe and Mail, Canada’s national newspaper, a few weeks ago. There was little extraordinary about his death. He was a widower, had suffered from multiple health problems, and had been on kidney dialysis for 18 months. Considered to be too ill to qualify for a transplant, he decided to end dialysis. He died in a hospice in a Toronto suburb.
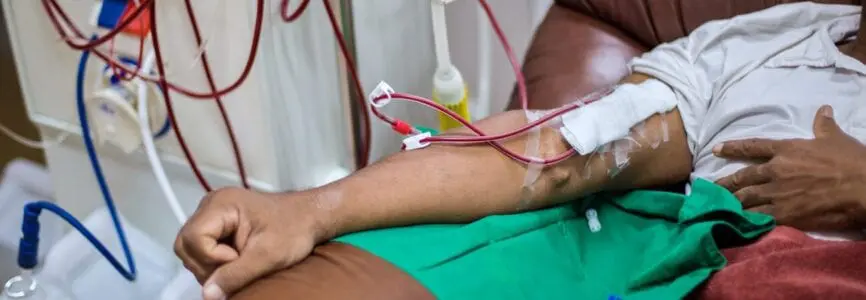
Two aspects of Mr. Drier’s death seem worth putting on record for bioethicists to remember. The first is the burden of dialysis. Mr. Drier had the unusual job of designing exterior walls for skyscrapers, and that explains how he describes dialysis. “I’ve stood 790 feet in the air on bamboo scaffolding,” he’s quoted as saying, “Not a whole lot has scared me. One thing I have a phobia about—that just turns me into Jell-O, I can’t stand it—is needles.” He then compares his experience of dialysis to someone with a phobia of snakes. “Here, hold this snake four hours a day, three days a week,” he says.
The Globe quotes a nephrologist saying that while some patients “tolerate the procedure well and are grateful for the extra years it gives them . . . others find it diminishes them, body and soul.” When I think about autonomy in treatment decisions, I want to remember Mr. Drier’s analogy of holding the snake.
The second issue on which I find Mr. Drier to be eloquent is dependency. I read some ethicists writing about people’s “fear of dependency” as if this were some sort of individual psychopathology, encouraged by societal stigmatization. Mr. Drier refuses prolonged, terminal dependency for reasons that pretty well describe how I’ve imagined the responsibility of parenthood in my life. Here’s what he told the newspaper: “My kids are like, ‘Dad, we’ll tear our lives apart and live with you and take care of you.’ I spent 30 years getting them to the point they’re at. Why on Earth would I do that to them? And for what purpose? To extend my miserable and painful existence?”
The word responsible gets tossed around a lot in discussions of choices in dying. For me, Mr. Drier’s death exemplifies what responsible means. His sense of responsibility explains why he would say that “God blessed me with kidney failure, because it’s an on and off switch.” Not every disease offers that switch, and responsibility demands that we negotiate multiple factors: available care facilities, medical options, legal context. I think not in principles but in fragments of stories. Mr. Drier’s “Why on Earth would I do that to them?” is a fragment I want to hold onto.
Arthur Frank is professor emeritus at the University of Calgary and a Fellow of The Hastings Center. His blog is found at arthurwfrank.wordpress.com.













I like so much the article! Agree totally
Gisela Farias
Thank you for this beautiful essay. In the interest of perhaps unnecessarily complicating a reasonable decision to forego burdensome medical care, I offer the following assertion by the 12th century Jewish philosopher/legal scholar/physician Maimonides (as quoted in an essay by the late Jewish philosopher rabbi David Hartman). A man “who cannot live without help but who, in his pride, declines to accept help is a shedder of blood, guilty of attempts on his own life.”
Maimonides was likely referring to willingness to accept charity here, rather than mandating unending kidney dialysis, and even regarding the decision to accept charity he wrote elsewhere that a person should be somewhat reluctant to accept it for fear of falling into dependency. Regarding Paul Drier, I agree with Arthur Frank that his doctors and family ought best to have supported him in his decision, and that bioethicists ought not label him and others like him who decide to stop life prolonging medical treatment as suffering from irrational fear of dependency. But I would also understand Maimonides as asking us to interrogate Drier’s unwillingness to continue dialysis, rather than simply accept that refusal at face value. Had I been his doctor, I would have wanted to continue the conversation about his decision without pressuring him in any way, making sure that he understood that he was loved and that no one considered him a burden. I’d want to be certain that stopping dialysis was what he wanted, that if phobia of needles was the issue, that there was nothing I could do to alleviate that phobia, and give the decision the necessary time. Admittedly it’s a fine line and a delicate conversation.
A number of philosophical and religious traditions are backing off of the traditional judgment that extraordinary modes of treatment ethically may be forgone if the patient balks at them. I realize that the ordinary / extraordinary line is hard to draw. To me, it has less utility as a clinical criterion than as an indicator of patient suffering, of an unfavorable proportionality judgment on his or her part. Mr. Drier may have been struggling to express some such concern. Thanks to Prof. Frank for raising this troubling case to our attention.
My mother accepted an indwelling dialysis setup, under some pressure from the doctors and, I am sorry to say, to some extent me. I saidto her that she could always ask them to take it out again if it proved unacceptable, but that is much easier said than done. The sensations from the apparatus, and her knowledge and imagining of what it was doing gave her the heebie jeebies, and kept her awake and ill at ease. It was not an acceptable life.