Hastings Center News
For Medicare Coverage, What Outcomes Should Count and What Evidence Is Needed?
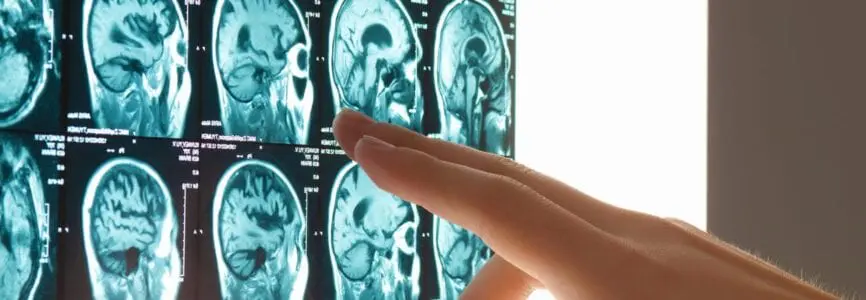
Why doesn’t Medicare pay unconditionally for amyloid PET imaging, a brain scan that identifies whether patients have beta amyloid plaque in their brain tissue, which may be a contributing factor for Alzheimer’s disease? This question is at the heart of current disputes about health technology assessment for regulatory approval and payer coverage of new medical technologies. It is examined in detail in an article by Hastings Center research scholars Karen Maschke and Michael Gusmano in the Journal of Aging & Social Policy.
Many scientists argue that amyloid plaque in the brain may be a biomarker for Alzheimer’s disease, though recent Alzheimer’s drug trials have failed to confirm this hypothesis. Nonetheless, there is evidence that amyloid plaque plays some role in Alzheimer’s disease. Until the availability of amyloid PET imaging, seeing amyloid plaque in a person’s brain was possible only at autopsy. Even though no treatments are available to forestall progression of Alzheimer’s disease, many physicians and patients argue that the information from amyloid PET imaging can be used to differentiate types of dementia in patients with cognitive decline. The “value of knowing” for patients and their families about the presence of amyloid plaque is also cited as a reason that Medicare should pay for the brain scan.
However, the Centers for Medicare and Medicaid Services (CMS) claimed that the evidentiary standard for whether a diagnostic test meets the statutory requirement of “reasonable and necessary” should be whether the use of that diagnostic test leads to improved patient outcomes in the Medicare population. Maschke and Gusmano point out that although stakeholders who wanted CMS to pay for amyloid PET imaging cited studies showing a benefit from this imaging technology, CMS said that most of those studies focused on test characteristics, not on patients’ health outcomes. Currently, CMS will only pay for amyloid PET imaging when Medicare patients are enrolled in clinical trials that meet certain criteria.
The decision elicited widespread disappointment. At an international Alzheimer’s Association conference, one clinician said that it posed a “moral dilemma” to those who want to help patients and families, according to Maschke and Gusmano. Three patients filed a lawsuit against CMS, with funding from one of the manufacturers of the imaging technology.
“Public and private insurers are increasingly asking for evidence that medical technologies are effective in improving patient health outcomes before they agree to pay for those technologies,” write Maschke and Gusmano. But, as the amyloid PET imaging decision illustrates, there remains considerable disagreement about what outcomes are relevant, and what standards of evidence should be used to evaluate those outcomes.