Bioethics Forum Essay
Charlie Gard, Compassionate Use, and Single-Payer Health Care
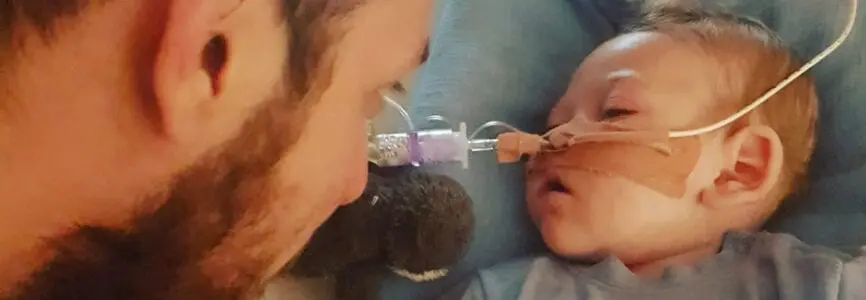
The case of Charlie Gard continued to unfold this week as Charlie’s parents, Connie Yates and Chris Gard, withdrew their appeal for permission to bring him to the United States for experimental treatment. The move came after tests showed that Charlie had sustained irreversible muscle damage, making recovery unlikely.
The international controversy began when doctors at Great Ormund Street Hospital concluded that there were no further interventions that were likely to help Charlie, who suffers from mitochondrial DNA depletion syndrome, and that extending his life further would cause him unnecessary suffering. Instead, they recommended palliative care. His parents, on the other hand, had argued that they could try using an experimental drug called nucleoside bypass therapy, which has not been tested in clinical trials. Under British law, cases like Charlie’s are resolved by the courts, and the High Court, the Court of Appeals, and the European Court of Human Rights each ruled that Charlie’s life support should be withdrawn. His parents now recognize that there is nothing more that could be done to help Charlie, and will try to spend as much time with him as they can in his final days.
Charlie’s case has sparked international debates on a host of ethical and political issues, especially over the ethics, advantages, and disadvantages of different health care systems. Many people have seized on the case as the epitome of the potential horrors of nationalized, single-payer health care systems. They claim that Charlie Gard is not receiving further treatment because the government decided not to pay for it, and that’s because the U.K.’s National Health Service doesn’t have the funds to take care of everyone.
It is true that at this time, the National Health Service will not pay for experimental treatments. However, this is not because the U.K. uses a nationalized, single-payer health care system. The American health care system has a similar policy.
In the United States, patients can apply to drug companies and the Food and Drug Administration to use unproven drugs under Compassionate Use or Expanded Access exceptions to the traditional drug approval processes. The idea behind compassionate use is that if patients are out of options, they should be allowed to try experimental medications if they are willing to accept the risk of unknown, severe side effects.
However, such medications are not traditionally covered by insurance: individuals must either raise their own funds, as Charlie’s parents did through GoFundMe, or hope that the drug companies will cover the cost of treatment. Although the FDA approves over 90% of Compassionate Use Applications, convincing companies to give patients the drugs is very difficult, since companies usually must cover the cost of the treatments. This can be difficult for small companies, which might drive themselves out of business without even getting closer to FDA approval.
Charlie’s case is somewhat different than compassionate use cases in America, in that the courts had also ordered the child’s life support to be withdrawn. However, as with the experimental medication, the reason was not financial, but because the doctors and courts believe that keeping Charlie alive is causing him needless suffering.
The Charlie Gard case indeed raises many significant questions about the role of the state in medical decision-making, the interests of family members, and the ethics of using experimental medications. However, it is important to remember that Charlie’s medical and financial situation would likely be the same, or even worse, in many countries throughout the world, regardless of whether they utilize a single-payer health care system.
Michael S. Dauber has served as a clinical ethicist and currently works on an institutional review board.













Thanks Michael. Wish you had gone even further. We all need a stiffer backbone to withstand expensive, futile treatment at the public expense. More importantly, we all need softer hearts for the bereaved who lose their dreams, hopes, meaning, and self-identity in relation to loved ones whose mortality comes too soon. Most especially for first time parents whose infant appears so cute and adorable on the surface. Appropriate and helpful end-of-life and spiritual counseling, as well as arms around love for the parents by the child’s care-givers are the low dollar high cost remedy. Have we forgotten that the emotional costs of high touch comes with the high costs of high tech? Why do empathy, sympathy, and comfort of shared loss and grief not come from human medical providers?
Thank you Michael for sharing your views on baby Charlie Guard. It is indeed very sad for his parents and certainly for many of us, by way of the media, came to know about this case. My friend asked for my views since I have to deal with many clinical ethical cases and my answer to her was accepting and letting go would be kinder. Moreover, we don’t know and would have difficulty appreciating how Charlie might suffer. Yet letting go is usually the most difficult thing to do for many clinicians and families, despite counseling and support. In this case, the Great Ormond Street Hospital is clear but the family is not, in some ways influenced by external societal pressure and politics. I agree with you that regardless of whatever payer system, Charlie’s financial status would not change. But, it most certainly has to be borne by someone else – often the taxpayers and perhaps some other organizations. Financial issue aside, are we missing something here about Charlie’s medical condition and Great Ormond Street’s professional judgment and decision? Seems to me like Professional judgment is important but keeping Charlie alive appears more so …